Every year, thousands of American adults experience the life-changing effects of shoulder fractures, yet many never realize how complex these injuries can be. For those in Austin, understanding the differences between a fracture, dislocation, or soft tissue damage is vital for a swift recovery. Whether you are healing from a fall or high-impact accident, this guide uncovers the truth about shoulder fractures, clears up common myths, and explains why fellowship-trained orthopedic care truly matters.
Table of Contents
- Shoulder Fractures Defined and Common Myths
- Major Types of Shoulder Fractures Explained
- How Orthopedic Specialists Diagnose Fractures
- Treatment Options for Each Fracture Type
- Risks, Recovery Time, and Functional Outcomes
Key Takeaways
| Point | Details |
|---|---|
| Understanding Fractures | Shoulder fractures vary significantly in type, location, and treatment approaches, highlighting the need for expert evaluation. |
| Diagnosis Importance | A thorough diagnostic process including patient history and advanced imaging is crucial for accurate treatment planning. |
| Tailored Treatment | Treatment strategies must be customized based on the fracture type, patient characteristics, and potential complications. |
| Recovery Dynamics | Recovery timelines can vary, emphasizing the importance of following rehabilitation protocols for optimal outcomes. |
Shoulder Fractures Defined and Common Myths
Shoulder fractures represent complex orthopedic injuries involving breaks in the shoulder’s intricate bone structure, typically caused by high-impact trauma such as vehicle accidents or significant falls. Understanding shoulder fracture characteristics requires recognizing the unique anatomy of this critical joint, which comprises three primary bones: the clavicle, proximal humerus, and scapula.
Contrary to popular misconceptions, shoulder fractures are not simply equivalent to dislocations or soft tissue injuries. Each type of shoulder fracture presents distinct symptoms and treatment protocols. Bone displacement, pain intensity, and mobility limitations vary significantly depending on which specific shoulder bone sustains the fracture. For Austin patients, professional medical assessment becomes crucial in determining the precise injury type and developing an appropriate recovery strategy.
The most common shoulder fracture myths include believing all shoulder injuries heal identically or that immobilization alone guarantees complete recovery. In reality, shoulder trauma requires specialized medical evaluation to prevent long-term complications. Factors like patient age, fracture location, and overall health significantly influence treatment approaches, which might range from conservative methods like bracing to surgical intervention.
Pro tip: Always seek professional orthopedic consultation within 48 hours of a suspected shoulder fracture to ensure proper diagnosis and prevent potential long-term mobility restrictions.
Major Types of Shoulder Fractures Explained
Shoulder fractures are classified into three primary types based on the specific bone involved: the clavicle (collarbone), scapula (shoulder blade), and proximal humerus (upper arm bone). Shoulder fracture classification helps orthopedic specialists develop targeted treatment strategies that address the unique characteristics of each bone injury.
The clavicle fracture is the most frequently encountered shoulder fracture, often characterized by a visible bump and potential shoulder sagging. These fractures typically result from direct impact or falls and can cause significant discomfort for patients. The proximity to major nerves and blood vessels means careful medical evaluation is crucial to prevent potential complications.
Scapula fractures represent a rare but complex injury type, accounting for less than 1% of all fractures. The scapula’s robust muscular protection makes these fractures uncommon and usually indicative of high-energy trauma. The fracture location within the scapula—whether involving the glenoid, acromion, or coracoid process—determines the specific treatment approach and potential surgical intervention requirements.
The proximal humerus fracture presents significant variability in severity and complexity. These fractures can be displaced or nondisplaced, with treatment options ranging from conservative management to surgical reconstruction. Factors such as patient age, bone quality, and the specific fracture pattern play critical roles in determining the most appropriate treatment strategy.

Pro tip: Request a detailed imaging study like CT scan or MRI to understand the precise fracture pattern and potential soft tissue involvement when consulting an orthopedic specialist.
Here’s a side-by-side comparison of the three major shoulder fracture types, highlighting their defining features and treatment challenges:
| Fracture Type | Frequency | Key Features | Main Treatment Challenges |
|---|---|---|---|
| Clavicle | Most common | Visible bump, shoulder sag | Proximity to nerves and vessels |
| Scapula | Very rare | Protected by muscles, complex | High-energy trauma, surgical need |
| Proximal Humerus | Variable severity | Displaced or nondisplaced | Bone quality, fracture pattern |
How Orthopedic Specialists Diagnose Fractures
Diagnosing shoulder fractures requires a comprehensive, multi-step approach that combines patient history, physical examination, and advanced imaging techniques. Orthopedic diagnostic protocols are designed to precisely identify the nature, location, and extent of shoulder bone injuries, ensuring accurate treatment planning for Austin patients.
The diagnostic process begins with a detailed patient history and thorough physical examination. Specialists carefully assess pain levels, shoulder deformity, and range of motion while checking for specific indicators of fracture. Physical assessment involves gentle palpation to identify areas of tenderness, swelling, or unusual bone alignment. Orthopedic experts look for visual signs like bruising, asymmetry, and ask about the specific mechanism of injury to understand the potential fracture pattern.
Imaging studies form the cornerstone of shoulder fracture diagnosis. Standard X-rays provide initial insights into bone structure and fracture location, while more complex cases might require advanced imaging. Computed Tomography (CT) scans offer detailed three-dimensional views of bone disruption, helping specialists understand intricate fracture patterns. Magnetic Resonance Imaging (MRI) becomes critical when assessing potential soft tissue damage, such as injuries to the rotator cuff or surrounding ligaments that might accompany the fracture.
Followup imaging plays a crucial role in monitoring healing progression. Orthopedic specialists use sequential X-rays to track bone alignment, assess healing rates, and determine whether the fracture is responding to the chosen treatment strategy. This ongoing monitoring allows for dynamic adjustment of rehabilitation protocols and ensures optimal recovery for patients.
Pro tip: During your initial consultation, request copies of all diagnostic imaging to maintain a personal medical record and facilitate comprehensive understanding of your shoulder injury.
Below is a summary of imaging techniques used in shoulder fracture diagnosis, with their unique advantages:
| Imaging Method | Best for Detecting | Advantages |
|---|---|---|
| Standard X-ray | Bone breaks, alignment issues | Quick and widely available |
| CT Scan | Complex fracture patterns | Detailed 3D bone views |
| MRI | Soft tissue involvement | Identifies ligament, tendon damage |
| Followup X-ray | Healing progress and alignment | Monitors recovery over time |
Treatment Options for Each Fracture Type
Shoulder fracture treatment strategies demand a nuanced approach tailored to the specific bone involved, injury severity, and individual patient characteristics. Understanding the unique treatment requirements for each fracture type helps Austin patients navigate their recovery with confidence and clarity.
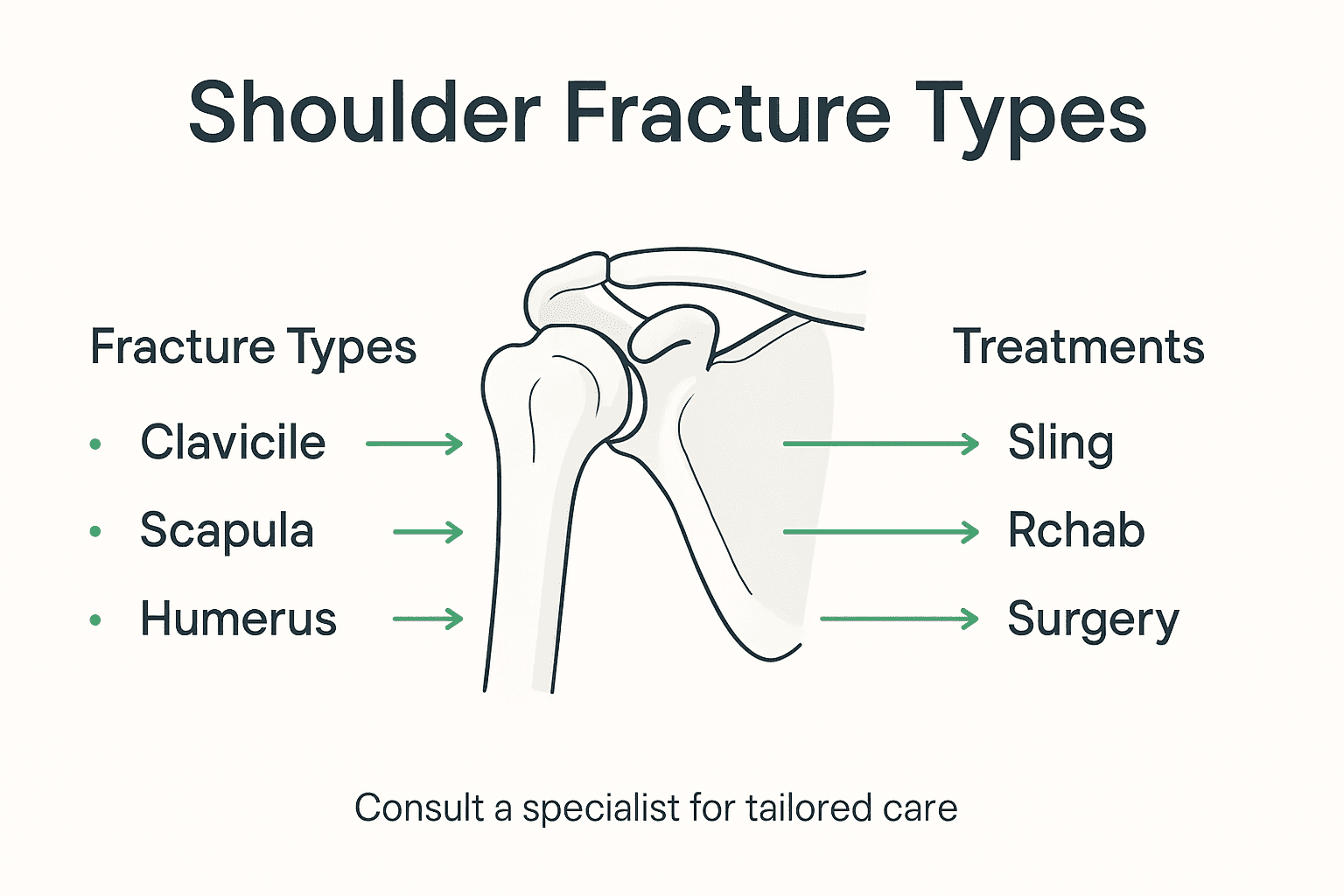
For clavicle fractures, treatment typically begins with conservative management. Most patients will receive a supportive sling to immobilize the shoulder and promote natural healing. Significantly displaced fractures, however, may require surgical intervention involving plate and screw fixation to restore proper bone alignment and prevent long-term mobility restrictions. The decision between surgical and nonsurgical approaches depends on factors like fracture complexity, patient age, and overall physical activity level.
Scapula fractures present a unique challenge for orthopedic specialists. These rare injuries usually respond well to nonoperative care, with treatment focused on pain management and limited activity. A comprehensive approach involves initial immobilization using a shoulder sling, followed by carefully structured rehabilitation. In complex cases involving significant glenoid displacement, surgical reconstruction might become necessary to ensure proper joint function and prevent potential long-term complications.
Proximal humerus fractures represent the most variable injury type, with treatment options ranging from simple immobilization to complex surgical reconstruction. Minor, nondisplaced fractures can often heal with conservative methods like sling immobilization and progressive physical therapy. More severe fractures might require advanced surgical techniques, including internal fixation with plates and screws or, in extreme cases, partial or total shoulder replacement. The specific treatment protocol depends on factors such as bone fragment displacement, patient age, bone quality, and overall health status.
Pro tip: Request a comprehensive rehabilitation plan from your orthopedic specialist that includes specific milestones and progressive mobility exercises tailored to your specific fracture type and healing progress.
Risks, Recovery Time, and Functional Outcomes
Shoulder fracture recovery dynamics represent a complex journey that varies significantly based on individual patient factors and specific injury characteristics. Understanding the potential risks, expected recovery timelines, and functional outcomes helps Austin patients set realistic expectations and actively participate in their healing process.
The typical recovery timeline spans six to nine months, with the first six to eight weeks focused on immobilization using specialized shoulder slings. Healing progression involves multiple critical stages, including initial stabilization, gradual movement restoration, and comprehensive rehabilitation. Potential risks during this period include developing stiffness, muscle weakness, nonunion of bone fragments, and potential nerve complications that could impact long-term shoulder functionality.
Proximal humerus fractures often present the most complex recovery scenario. Surgical intervention may be necessary to improve functional outcomes, particularly for patients experiencing significant bone displacement or those with underlying medical conditions. Factors such as patient age, overall health status, and adherence to rehabilitation protocols dramatically influence the final functional result. Some patients may experience reduced range of motion, while others can achieve near-complete shoulder mobility with dedicated physical therapy.
Postoperative rehabilitation represents a critical component of shoulder fracture recovery. Patients should expect a graduated approach that begins with gentle movements and progressively increases in complexity. Physical therapists work closely with orthopedic specialists to design individualized recovery plans that address specific injury characteristics, minimize potential complications, and restore optimal shoulder function.
Pro tip: Document your recovery progress through photographs and detailed notes to help your medical team track healing and adjust rehabilitation strategies effectively.
Expert Care for Your Shoulder Fracture Recovery Starts Here
Shoulder fractures can feel overwhelming with their complex types and varied treatment options. Whether you are dealing with a clavicle fracture causing visible discomfort or a challenging proximal humerus injury requiring surgery, understanding your path to recovery is key. At Hand To Shoulder Austin, we know how critical personalized care and precise diagnosis are to restoring your shoulder’s strength and mobility. Our fellowship-trained, board-certified surgeon Dr. Manish V. Patel specializes in creating customized treatment plans that address the unique nature of your fracture and healing needs.
Take control of your healing journey by exploring our Surgery Recovery & Rehab Guides | Austin Orthopedic Care for tailored rehabilitation strategies. For athletes or active individuals facing shoulder trauma, our insights at Sports Medicine & Athlete Care | Austin Orthopedic Blog provide essential tips to speed recovery and prevent reinjury. Don’t wait for complications or limited mobility to set in. Schedule your evaluation today at Hand To Shoulder Austin and start the path toward confident movement and lasting shoulder health.
Frequently Asked Questions
What are the main types of shoulder fractures?
Shoulder fractures are primarily classified into three types: clavicle fractures, scapula fractures, and proximal humerus fractures. Each type has unique characteristics and treatment strategies.
How is a shoulder fracture diagnosed?
A shoulder fracture is diagnosed through a comprehensive approach that includes patient history, physical examination, and advanced imaging techniques like X-rays, CT scans, and MRIs to assess the injury’s extent.
What are the common symptoms of a shoulder fracture?
Common symptoms of a shoulder fracture include intense pain, visible deformity, swelling, bruising, and limited range of motion in the affected shoulder.
What is the typical recovery time for a shoulder fracture?
The recovery time for a shoulder fracture typically spans six to nine months, with initial immobilization lasting six to eight weeks, followed by rehabilitation to restore movement and strength.