Every year, more than 50,000 American adults undergo shoulder joint replacement surgery to reclaim pain free movement and independence. For those struggling with chronic pain or severe joint damage, finding a safe path back to an active lifestyle is a major priority. Discover how recent advances in procedure types, recovery techniques, and physician expertise are transforming outcomes for American patients facing shoulder joint replacement.
Table of Contents
- What Shoulder Joint Replacement Involves
- Types of Shoulder Replacement Procedures
- How Surgery Works and Who Qualifies
- Recovery Process and Patient Expectations
- Risks, Complications, and Alternatives
Key Takeaways
| Point | Details |
|---|---|
| Shoulder Joint Replacement Purpose | This surgical procedure aims to restore mobility and alleviate chronic pain in patients with severe shoulder joint damage. |
| Types of Procedures | The main techniques include Anatomic Total, Reverse Total, and Partial Shoulder Replacement, each tailored to specific patient conditions. |
| Recovery Expectations | Post-surgery recovery involves a structured rehabilitation process, typically lasting 3-6 months, with full recovery potentially taking up to one year. |
| Risks and Alternatives | Patients should be aware of surgical risks such as infection and consider alternative treatments like PRP therapy and physical therapy before opting for surgery. |
What Shoulder Joint Replacement Involves
Shoulder joint replacement is an advanced surgical procedure designed to restore mobility and reduce chronic pain for patients experiencing severe shoulder joint damage. This intricate surgical intervention involves removing damaged portions of the shoulder joint and replacing them with artificial components crafted from high grade medical metals and durable polymers.
The surgical process typically begins with a comprehensive evaluation of the patient’s shoulder anatomy, medical history, and specific joint damage. During the procedure, an orthopedic surgeon like Dr. Manish V. Patel will carefully remove damaged bone and cartilage from the shoulder’s ball and socket joint. Precision is critical – surgeons use specialized instruments to prepare the remaining bone surfaces to receive prosthetic components that will mimic natural joint mechanics.
The prosthetic shoulder joint generally consists of two primary components: a metal ball that replaces the damaged humeral head, and a plastic socket that substitutes for the damaged shoulder socket (glenoid). These components are meticulously designed to provide smooth, pain free movement and restore range of motion. Modern shoulder replacement technologies have advanced significantly, offering patients improved surgical techniques that minimize recovery time and maximize functional outcomes.
PRP (Platelet Rich Plasma) therapy can also play a crucial role in supporting recovery after shoulder joint replacement, helping accelerate healing and reduce inflammation during the rehabilitation process. Patients can expect a structured recovery program that typically involves physical therapy, gradual movement restoration, and careful monitoring to ensure optimal joint function.
Pro Tip: Schedule multiple follow up consultations with your orthopedic surgeon to track your shoulder joint replacement recovery progress and address any concerns promptly during the healing process.
Types of Shoulder Replacement Procedures
Shoulder replacement procedures are complex surgical interventions designed to address different types of shoulder joint damage and patient needs. Shoulder replacement techniques have evolved significantly, offering specialized options tailored to individual patient conditions and anatomical requirements.
Two primary shoulder replacement approaches dominate contemporary orthopedic practice: Anatomic Total Shoulder Replacement and Reverse Total Shoulder Replacement. Anatomic total shoulder replacement mimics the natural shoulder anatomy, using prosthetic components that replicate the original joint structure. This technique is typically recommended for patients with intact rotator cuff muscles and relatively straightforward joint deterioration. Surgeons carefully select this approach when the patient’s existing shoulder biomechanics can support traditional joint replacement.
Reverse total shoulder replacement represents a more specialized intervention, fundamentally redesigning joint mechanics to compensate for significant rotator cuff damage. In this procedure, the socket and ball components are strategically switched – the metal ball is attached to the shoulder blade (scapula), while the plastic socket is fitted to the upper arm bone (humerus). This innovative technique provides enhanced stability and function for patients with complex shoulder conditions, particularly those experiencing severe rotator cuff tears or advanced arthritis that compromises standard joint replacement strategies.
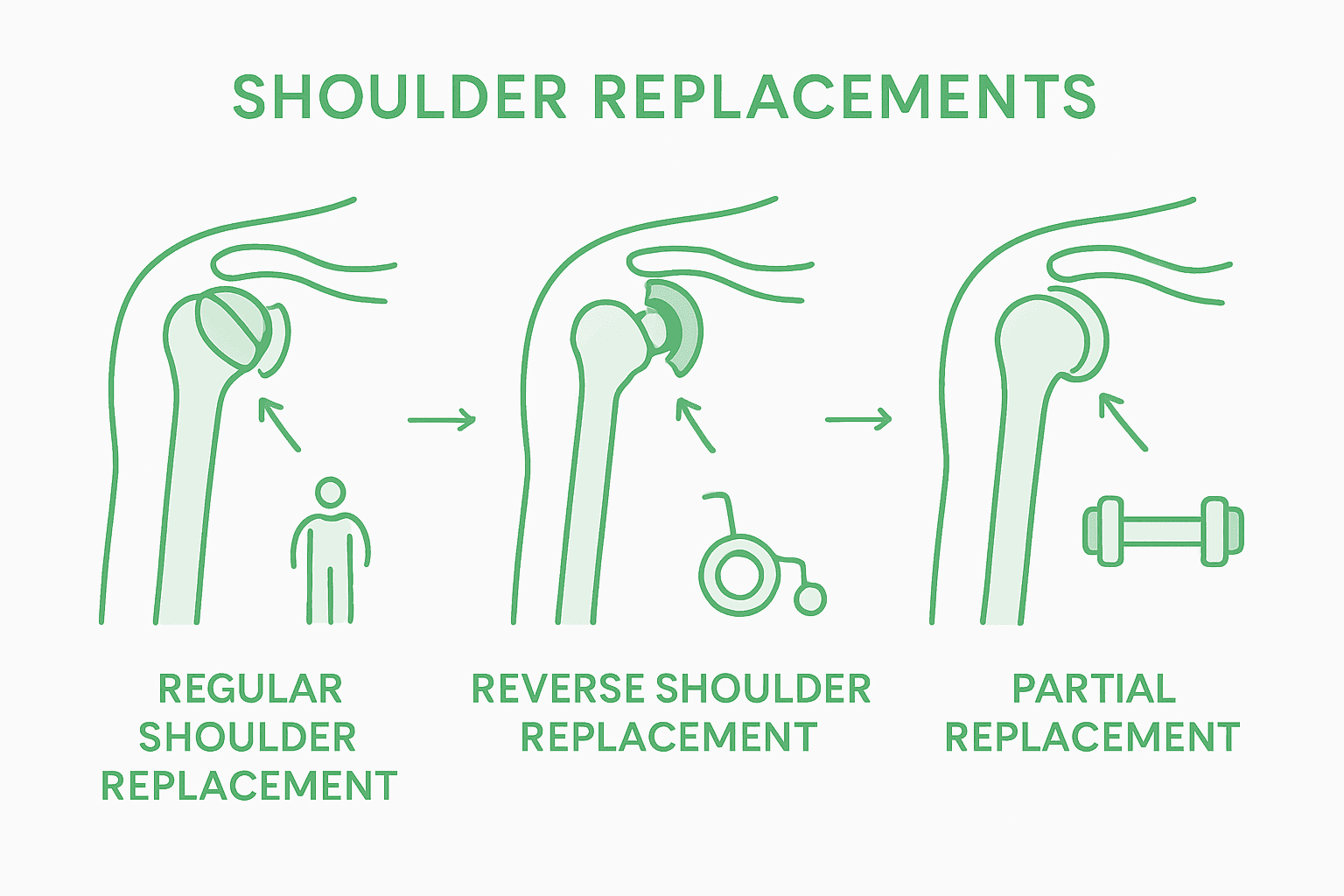
A third, less common option is Partial Shoulder Replacement, which involves replacing only the damaged portion of the shoulder joint. This approach is typically utilized when damage is localized and extensive total joint replacement is not yet necessary. Each replacement technique requires meticulous surgical planning, precise execution, and personalized rehabilitation strategies.
Here’s a concise comparison of main shoulder replacement procedures and their typical uses:
| Procedure Type | Primary Use Case | Key Surgical Feature |
|---|---|---|
| Anatomic Total Shoulder | Intact rotator cuff | Mimics natural joint anatomy |
| Reverse Total Shoulder | Severe cuff damage | Switches ball and socket positions |
| Partial Shoulder Replacement | Localized joint damage | Only replaces damaged joint portion |
Pro Tip: Request a comprehensive preoperative consultation to understand which shoulder replacement procedure best matches your specific shoulder condition and long term functional goals.
How Surgery Works and Who Qualifies
Shoulder joint replacement surgery is a complex medical procedure designed to restore function and alleviate chronic pain for patients with severe shoulder joint deterioration. Understanding surgical candidacy requires a comprehensive evaluation of multiple medical and lifestyle factors that determine whether a patient is an ideal candidate for this transformative intervention.
Qualification for shoulder joint replacement typically involves several critical considerations. Chronic Pain emerges as the primary indicator, specifically persistent discomfort that significantly impairs daily activities and does not respond to conservative treatments like physical therapy, medication, or PRP (Platelet Rich Plasma) injections. Patients experiencing limited shoulder mobility, substantial joint damage from conditions such as osteoarthritis, rheumatoid arthritis, or severe rotator cuff injuries are often the most suitable candidates for surgical intervention.
The surgical procedure itself involves intricate steps designed to minimize patient trauma and maximize functional recovery. Orthopedic surgeons begin with detailed preoperative imaging to map the precise anatomical requirements. During surgery, damaged joint surfaces are carefully removed and replaced with specialized prosthetic components. The procedure typically requires general anesthesia and can last between one to three hours, depending on the complexity of the individual case and the specific replacement technique being utilized.
Patient selection criteria extend beyond medical conditions and include comprehensive health assessments. Ideal candidates are generally individuals who are in reasonable overall health, do not have active infections, possess adequate bone quality to support prosthetic implantation, and demonstrate a commitment to post surgical rehabilitation. Age is less critical than overall health status, with successful surgeries performed on patients ranging from their 40s to 80s.
Pro Tip: Compile a detailed medical history and complete all recommended preoperative screenings to optimize your shoulder replacement surgery evaluation and potential success.
Recovery Process and Patient Expectations
Shoulder joint replacement recovery is a comprehensive journey that requires patience, dedication, and strategic rehabilitation. Recovery from shoulder replacement surgery demands a structured approach to regain strength, mobility, and functional independence.
The immediate postoperative period typically involves hospital monitoring for 1-2 days, during which pain management and initial mobility assessments are conducted. Patients will have their arm placed in a specialized sling to protect the surgical site and minimize joint stress. Pain Management becomes a critical focus, with physicians often utilizing a combination of prescribed medications, PRP (Platelet Rich Plasma) therapy, and targeted interventional techniques to control discomfort and support healing.
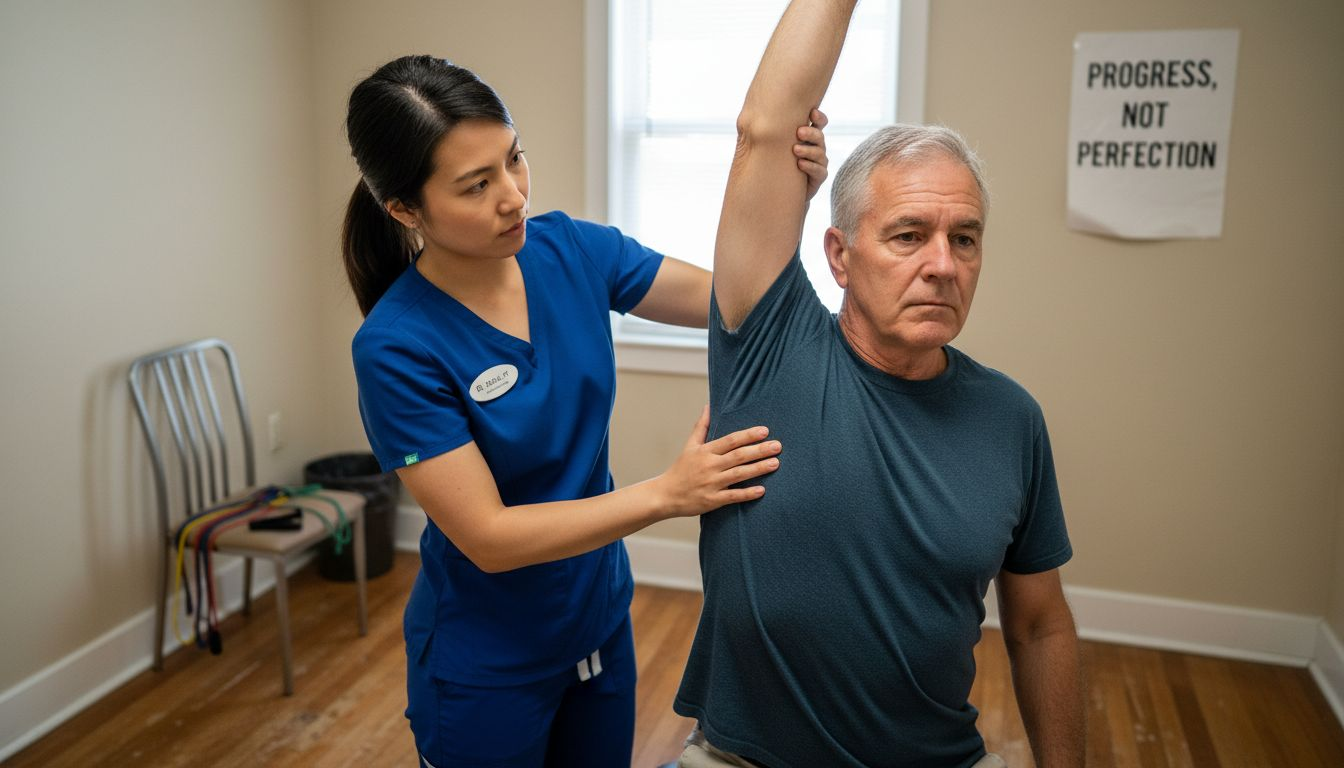
Physical therapy emerges as a cornerstone of successful shoulder replacement recovery. The rehabilitation process is typically divided into progressive stages, each designed to gradually restore range of motion and rebuild muscle strength. Initial therapy sessions focus on gentle movements and pain control, gradually advancing to more complex exercises that restore joint functionality. Patients can expect a comprehensive therapy program that might extend 3-6 months, with significant improvements typically observed within the first 12 weeks post surgery.
Patient expectations should be grounded in realistic timelines and personal commitment. Most individuals can anticipate returning to light activities within 6-10 weeks, with full recovery potentially taking up to one year. Factors such as age, overall health, adherence to rehabilitation protocols, and preexisting conditions can significantly influence individual recovery trajectories. Consistent communication with healthcare providers and active participation in prescribed rehabilitation exercises are crucial for optimal outcomes.
To better understand recovery, review these common phases after shoulder replacement:
| Recovery Phase | Typical Duration | Key Focus |
|---|---|---|
| Hospital Stay | 1-2 days | Pain control, monitoring |
| Initial Rehabilitation | 2-6 weeks | Gentle movement, healing |
| Functional Rehabilitation | 6-12 weeks | Strength, mobility build |
| Full Recovery | Up to 1 year | Return to daily activity |
Pro Tip: Document your recovery progress with detailed notes and photographs to help your medical team track healing and adjust rehabilitation strategies effectively.
Risks, Complications, and Alternatives
Shoulder joint replacement, while a transformative medical procedure, requires patients to understand potential risks and explore comprehensive treatment options. Understanding surgical risks is crucial for making informed healthcare decisions that align with individual medical needs and long term wellness goals.
Several potential complications can arise from shoulder joint replacement surgery. Surgical Risks include infection, blood clot formation, prosthetic component loosening, nerve damage, and limited range of motion. Infection represents the most serious potential complication, with risks ranging from superficial wound infections to deeper, more complex joint infections that might require additional surgical intervention. Blood clots pose significant concerns, particularly for patients with pre existing cardiovascular conditions or limited mobility during recovery.
Before pursuing surgical intervention, patients should carefully consider alternative treatment strategies. Conservative approaches like PRP (Platelet Rich Plasma) therapy can provide significant pain management and potential healing for certain shoulder conditions. Physical therapy, targeted exercise programs, anti inflammatory medications, and regenerative medicine techniques offer non surgical alternatives that might delay or potentially eliminate the need for complete joint replacement. These approaches are particularly effective for patients with early stage joint deterioration or those seeking less invasive treatment options.
Patients must engage in comprehensive consultations with orthopedic specialists to thoroughly evaluate their individual circumstances. Factors such as age, overall health status, activity level, and specific shoulder condition will significantly influence the recommended treatment pathway. Some patients might benefit from partial joint replacement or minimally invasive surgical techniques that preserve more of the natural joint structure, offering potentially faster recovery and reduced surgical trauma.
Pro Tip: Request a comprehensive diagnostic assessment that includes advanced imaging and a detailed discussion of both surgical and non surgical treatment options before making your final decision.
Take the Next Step Toward Restored Shoulder Mobility and Life After Surgery
If you are dealing with persistent shoulder pain or limited movement after shoulder joint replacement surgery, understanding your recovery journey and available treatment options is essential. This article highlighted challenges such as managing postoperative pain, optimizing physical therapy, and knowing what to expect during rehabilitation. At Hand To Shoulder Austin, we specialize in personalized orthopedic care tailored to your unique needs. Whether you need expert guidance on recovery or want to explore specific procedures including advanced shoulder replacements, our resources can help empower you.
Explore our Shoulder Surgery & Care Articles | Austin Orthopedic Blog for in-depth insights and proven strategies to support your healing process. Learn more about specialized issues such as rotator cuff involvement at Rotator Cuff Archives – Austin Hand To Shoulder. Take control of your shoulder health today by scheduling a consultation with Dr. Manish V. Patel who is dedicated to helping Austin patients achieve the best possible outcomes. Visit Hand To Shoulder Austin now to book your appointment and start your personalized treatment journey.
Frequently Asked Questions
What should I expect during the recovery process after shoulder joint replacement surgery?
The recovery process typically involves a hospital stay of 1-2 days, followed by a structured rehabilitation program that may last 3-6 months. Initial recovery focuses on pain management and gentle movements, gradually progressing to strength-building exercises.
How long does it take to fully recover from shoulder joint replacement surgery?
Full recovery can take up to one year, but many patients return to light activities within 6-10 weeks. Individual recovery times vary based on factors like age, overall health, and adherence to rehabilitation protocols.
What are the risks and complications associated with shoulder joint replacement surgery?
Potential risks include infection, blood clots, prosthetic component loosening, nerve damage, and limited range of motion. It’s important to discuss these risks with your orthopedic surgeon prior to surgery.
What alternative treatments are available before considering shoulder joint replacement?
Alternative treatments include physical therapy, PRP (Platelet Rich Plasma) therapy, targeted exercise programs, anti-inflammatory medications, and other non-surgical options that may help manage pain and improve function in the early stages of joint deterioration.