Most American adults are surprised to learn that more than 50 million people in the United States live with some form of arthritis. Shoulder arthritis does not only affect older adults, and its symptoms often disrupt daily life for people of all ages. Understanding the real causes and symptoms can clear up common confusion, help recognize early warning signs, and lead to faster, more effective care.
Table of Contents
- Defining Shoulder Arthritis And Common Misconceptions
- Types Of Shoulder Arthritis And Key Differences
- Causes And Risk Factors In Shoulder Arthritis
- Typical Symptoms And How Arthritis Progresses
- Treatment Options For Shoulder Arthritis Pain
- Avoiding Misdiagnosis And When To Seek Care
Key Takeaways
| Point | Details |
|---|---|
| Understanding Shoulder Arthritis | Shoulder arthritis involves the degeneration of joint cartilage and can affect individuals of all ages, not just the elderly. Conditions such as previous injuries or autoimmune disorders can contribute to its development. |
| Recognizing Symptoms | Key symptoms include progressive stiffness, reduced range of motion, and persistent pain, which may worsen with activity. Accurate diagnosis is crucial, as other conditions can mimic arthritis. |
| Types and Treatment Options | There are different types of shoulder arthritis, such as osteoarthritis and rheumatoid arthritis, each requiring tailored treatment approaches. Non-surgical methods like physical therapy are often recommended before considering surgery. |
| Importance of Seeking Care | Individuals should seek medical advice for persistent shoulder pain or dysfunction, as early intervention can prevent further joint deterioration. Comprehensive evaluations will help determine the appropriate treatment plan. |
Defining Shoulder Arthritis and Common Misconceptions
Shoulder arthritis is a complex condition involving progressive degeneration of joint cartilage, which leads to significant pain and restricted mobility. Arthritis of the shoulder represents more than just occasional discomfort – it represents a systematic breakdown of joint structures that can dramatically impact daily functioning.
Contrary to popular belief, shoulder arthritis is not exclusively an older person’s condition. Inflammation and cartilage loss can occur in younger individuals due to factors like previous joint injuries, repetitive stress, genetic predisposition, or autoimmune disorders. This means athletes, workers with repetitive motions, and even younger adults can experience shoulder arthritis symptoms.
The condition manifests through several key characteristics. Patients typically experience progressive joint stiffness, reduced range of motion, grinding sensations during movement, and persistent aching that worsens with activity. While many assume all shoulder pain indicates arthritis, other conditions like rotator cuff injuries can produce similar symptoms, making professional diagnostic assessment crucial.
Pro Tip for Shoulder Health: Schedule regular consultations with an orthopedic specialist who can perform comprehensive joint assessments and recommend targeted treatments like PRP therapy to manage early-stage arthritis progression.
Types of Shoulder Arthritis and Key Differences
Shoulder arthritis encompasses several distinct types, each with unique characteristics and progression patterns. Shoulder arthritis classifications reveal five primary variations that impact joint health and mobility differently: osteoarthritis, rheumatoid arthritis, post-traumatic arthritis, rotator cuff tear arthropathy, and avascular necrosis.
Osteoarthritis represents the most common form, characterized by gradual cartilage breakdown related to aging and wear. In contrast, rheumatoid arthritis is an autoimmune condition where the body’s immune system attacks joint linings, causing widespread inflammation. Post-traumatic arthritis develops following significant joint injuries, while rotator cuff tear arthropathy emerges from complex shoulder tendon damage that disrupts normal joint mechanics.

Avascular necrosis stands out as a particularly challenging variant, occurring when blood supply to the shoulder bone is interrupted, leading to bone tissue death. Each type presents distinct diagnostic challenges, requiring specialized imaging and comprehensive physical assessments to determine the most appropriate treatment strategy. Factors like pain intensity, range of motion limitations, and underlying health conditions play crucial roles in determining the specific arthritis type and potential intervention approaches.
Pro Tip for Shoulder Health: Work closely with an orthopedic specialist to undergo comprehensive diagnostic testing that can precisely identify your specific shoulder arthritis type, enabling more targeted and effective treatment strategies like PRP therapy.
Here’s a summary of the major types of shoulder arthritis and how they differ:
| Arthritis Type | Typical Cause | Common Symptoms | Progression Pattern |
|---|---|---|---|
| Osteoarthritis | Aging and joint wear | Stiffness, aching | Slow, years-long decline |
| Rheumatoid Arthritis | Autoimmune attack on joints | Swelling, pain | Symmetrical, can flare up |
| Post-Traumatic Arthritis | Previous injury or trauma | Pain, grinding | Worsens with time |
| Rotator Cuff Tear Arthropathy | Major tendon tears | Weakness, instability | Gradual functional loss |
| Avascular Necrosis | Interrupted blood supply | Severe pain, collapse | Rapid cartilage deterioration |
Causes and Risk Factors in Shoulder Arthritis
Shoulder arthritis causes are multifaceted, involving a complex interplay of biological, genetic, and environmental factors. While aging remains the primary contributor, numerous underlying mechanisms can accelerate joint deterioration. Factors like previous shoulder injuries, repetitive motion, genetic predisposition, and systemic health conditions significantly influence arthritis development.
Age-related changes represent the most fundamental risk factor. As individuals progress through middle age and beyond, cartilage naturally loses its resilience and cushioning properties. Athletes, manual laborers, and individuals with physically demanding occupations face heightened risks due to cumulative joint stress. Genetic inheritance plays a crucial role, with family history of arthritis dramatically increasing an individual’s likelihood of developing the condition.
Traumatic injuries can substantially accelerate arthritis progression. Rotator cuff tears, shoulder dislocations, and significant impact injuries create lasting structural changes that compromise joint integrity. Autoimmune conditions like rheumatoid arthritis further complicate shoulder joint health by triggering inflammatory responses that progressively damage cartilage and surrounding tissues. Metabolic disorders, obesity, and chronic inflammation also contribute to accelerated joint deterioration.
Pro Tip for Joint Health: Implement proactive strategies like regular low-impact exercises, maintaining healthy body weight, and seeking early professional evaluations to minimize shoulder arthritis risk and potentially slow its progression through targeted interventions like PRP therapy.
Typical Symptoms and How Arthritis Progresses
Shoulder arthritis symptoms represent a progressive deterioration of joint function characterized by distinctive stages of pain and mobility limitations. The initial phase typically begins with intermittent discomfort during specific movements, gradually evolving into more persistent and intense sensations that significantly impact daily activities.
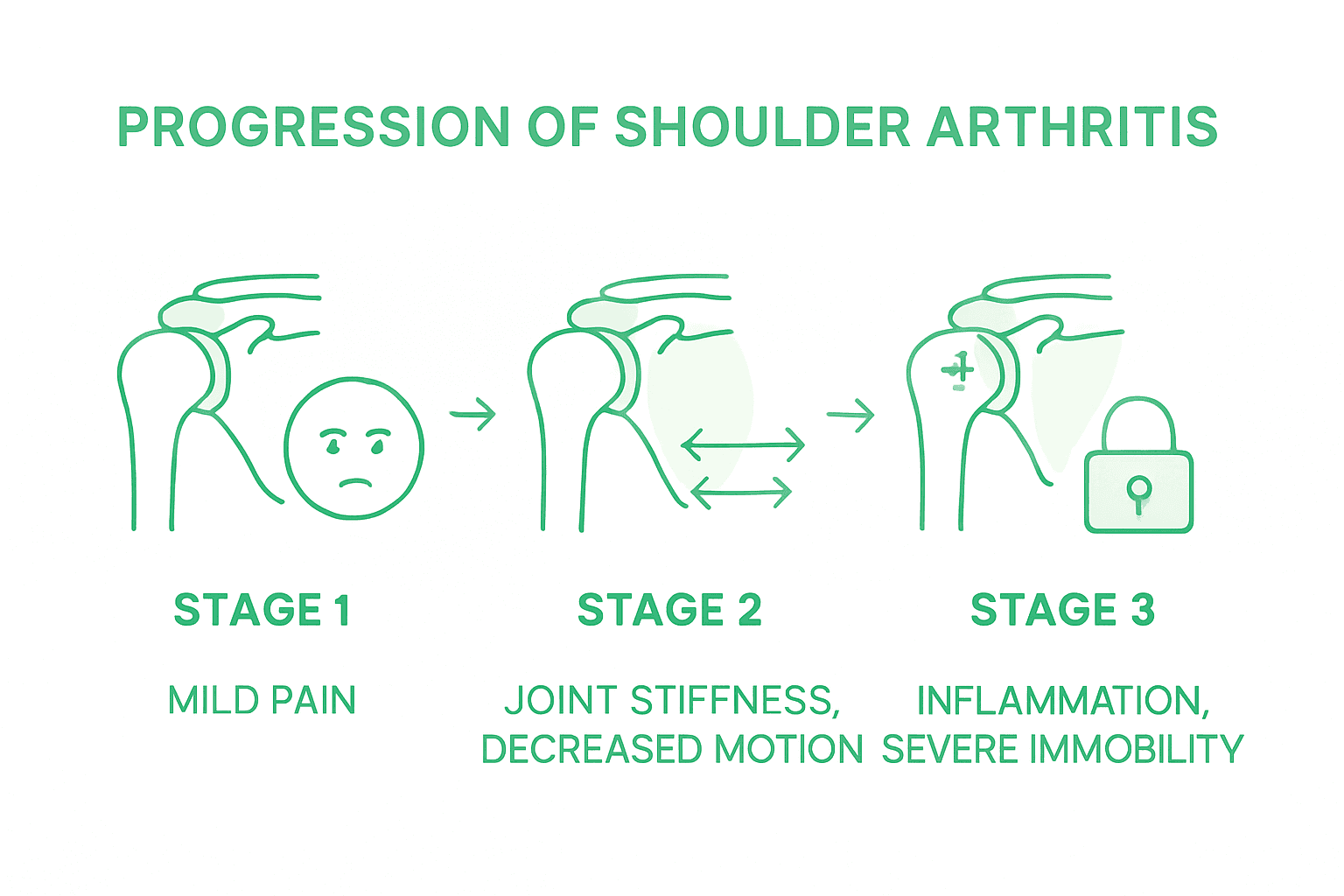
Pain patterns emerge as the primary indicator of arthritis progression. Early stages feature occasional aching during overhead movements or after extended physical activity. As the condition advances, patients experience more consistent pain that can occur both during movement and while at rest. The shoulder joint becomes increasingly stiff, with reduced range of motion making simple tasks like reaching, lifting, or even sleeping become challenging. Grinding or clicking sensations within the joint, known as crepitus, often develop as cartilage continues to degrade.
The advanced stages of shoulder arthritis introduce more severe functional limitations. Chronic inflammation leads to muscle weakness surrounding the joint, further compromising mobility and increasing overall discomfort. Bone spurs may develop, creating additional friction and pain during movement. Individuals might notice decreased strength in the affected arm, with activities requiring precise shoulder movements becoming progressively more difficult. Nighttime pain often increases, disrupting sleep and further impacting quality of life.
Pro Tip for Joint Management: Track your symptoms meticulously and consult an orthopedic specialist early to explore innovative treatment options like PRP therapy, which can potentially slow arthritis progression and manage pain more effectively.
Treatment Options for Shoulder Arthritis Pain
Shoulder arthritis treatment options range from conservative management strategies to advanced surgical interventions, designed to address pain, restore mobility, and slow disease progression. The approach depends on individual patient factors, including age, overall health, arthritis severity, and specific shoulder joint condition.
Non-surgical treatments form the initial management strategy. Physical therapy plays a crucial role, helping patients maintain joint flexibility and strengthen surrounding muscles. Targeted exercises and manual therapy techniques can reduce pain and improve range of motion. Medications like nonsteroidal anti-inflammatory drugs (NSAIDs) help manage pain and inflammation. Innovative treatments such as PRP therapy offer promising alternatives for patients seeking regenerative approaches that potentially stimulate tissue healing and reduce inflammatory responses.
In advanced cases where conservative treatments prove insufficient, surgical options become necessary. Procedures range from minimally invasive arthroscopic interventions to total shoulder replacement. Partial shoulder replacement might suit patients with localized joint damage, while total shoulder arthroplasty addresses widespread cartilage destruction. Emerging techniques like biological joint resurfacing and targeted cartilage regeneration represent cutting-edge alternatives that can provide more comprehensive long-term solutions for shoulder arthritis management.
Pro Tip for Treatment Selection: Collaborate closely with an orthopedic specialist to develop a personalized treatment strategy that considers your unique medical history, activity level, and specific arthritis progression, maximizing the potential for successful pain management and functional restoration.
Compare treatment strategies for shoulder arthritis at different severity stages:
| Stage | Non-Surgical Approaches | Surgical Options |
|---|---|---|
| Early | Physical therapy, NSAIDs, PRP therapy | Rarely required |
| Moderate | Exercise, injections, PRP | Arthroscopy or targeted procedures |
| Advanced | Pain management, limited exercise | Partial or total shoulder replacement |
Avoiding Misdiagnosis and When to Seek Care
Diagnosing shoulder arthritis requires careful medical evaluation to distinguish it from other shoulder conditions that produce similar symptoms. Conditions like rotator cuff injuries, bursitis, and tendonitis can mimic arthritis, making professional assessment crucial for accurate treatment planning.
Warning signs that demand immediate medical attention include persistent shoulder pain lasting more than a few weeks, significant restriction in range of motion, and pain that disrupts sleep or daily activities. Specific red flags include sharp pain during specific movements, audible grinding or clicking sounds in the joint, and progressive weakness in the shoulder and arm. Patients should be particularly vigilant if pain intensifies with activity and does not respond to rest, over-the-counter pain medications, or basic self-care strategies.
Professional diagnostic approaches involve comprehensive physical examinations, detailed medical history reviews, and advanced imaging techniques. X-rays, magnetic resonance imaging (MRI), and ultrasound can provide definitive insights into joint structural changes, cartilage degradation, and potential underlying conditions. Orthopedic specialists often conduct specific range-of-motion tests and assess pain responses to determine the exact nature and progression of shoulder joint deterioration. Additional diagnostic tools like blood tests might be employed to rule out autoimmune conditions that could be contributing to joint inflammation.
Pro Tip for Diagnostic Clarity: Document your symptoms meticulously, including pain location, intensity, duration, and specific movements that trigger discomfort, to provide your orthopedic specialist with comprehensive information for accurate diagnosis and targeted treatment planning.
Find Relief from Painful Shoulder Stiffness with Expert Arthritis Care
If you are struggling with the persistent stiffness and aching caused by shoulder arthritis you are not alone. This condition can limit your daily activities and reduce quality of life through progressive joint stiffness and grinding sensations as described in our detailed article. At the Austin Hand To Shoulder Center, we specialize in personalized treatment plans designed to address the unique challenges of shoulder arthritis including effective pain management and mobility restoration. Learn more about how innovative therapies and expert surgical options can improve your shoulder function in our Arthritis Treatment & Insights | Austin Hand To Shoulder Center section.
Take control of your shoulder health today by consulting with Dr Manish V Patel a fellowship-trained board-certified orthopedic surgeon dedicated to upper extremity care. Don’t wait for stiffness and pain to worsen visit the Austin Hand To Shoulder Center to schedule your appointment. Explore additional resources on maintaining joint health through our Sports Medicine & Athlete Care | Austin Orthopedic Blog and start your journey toward pain-free movement and improved function.
Frequently Asked Questions
What is shoulder arthritis and how does it cause pain?
Shoulder arthritis involves the degeneration of joint cartilage, leading to inflammation and significant pain, especially during movement. This deterioration restricts mobility, causing stiffness and discomfort in the shoulder joint.
What are the common symptoms of shoulder arthritis?
Common symptoms include progressive joint stiffness, reduced range of motion, persistent aching, and grinding sensations during movement. Patients often experience pain that worsens with activity and can impact daily activities.
How can I differentiate shoulder arthritis from other shoulder conditions?
Distinguishing shoulder arthritis from other conditions like rotator cuff injuries or tendonitis is essential. Key indicators include the type of pain, continuity of symptoms, and specific movements that exacerbate discomfort. A thorough medical evaluation is crucial for an accurate diagnosis.
What treatment options are available for shoulder arthritis?
Treatment options range from non-surgical methods like physical therapy and medication to surgical interventions, such as arthroscopy or shoulder replacement, depending on the severity of the condition. Consulting with an orthopedic specialist is vital for tailored treatment strategies.
Recommended
- Top Causes of Shoulder Pain—What Austin Patients Need to Know – Austin Hand To Shoulder
- Why Shoulder Pain Occurs – Causes and Impact – Austin Hand To Shoulder
- Frozen Shoulder Procedure: Complete Treatment Guide – Austin Hand To Shoulder
- Shoulder Pain in Athletes – Causes, Care, and Recovery – Austin Hand To Shoulder